Adverse Reactions | Vibepedia
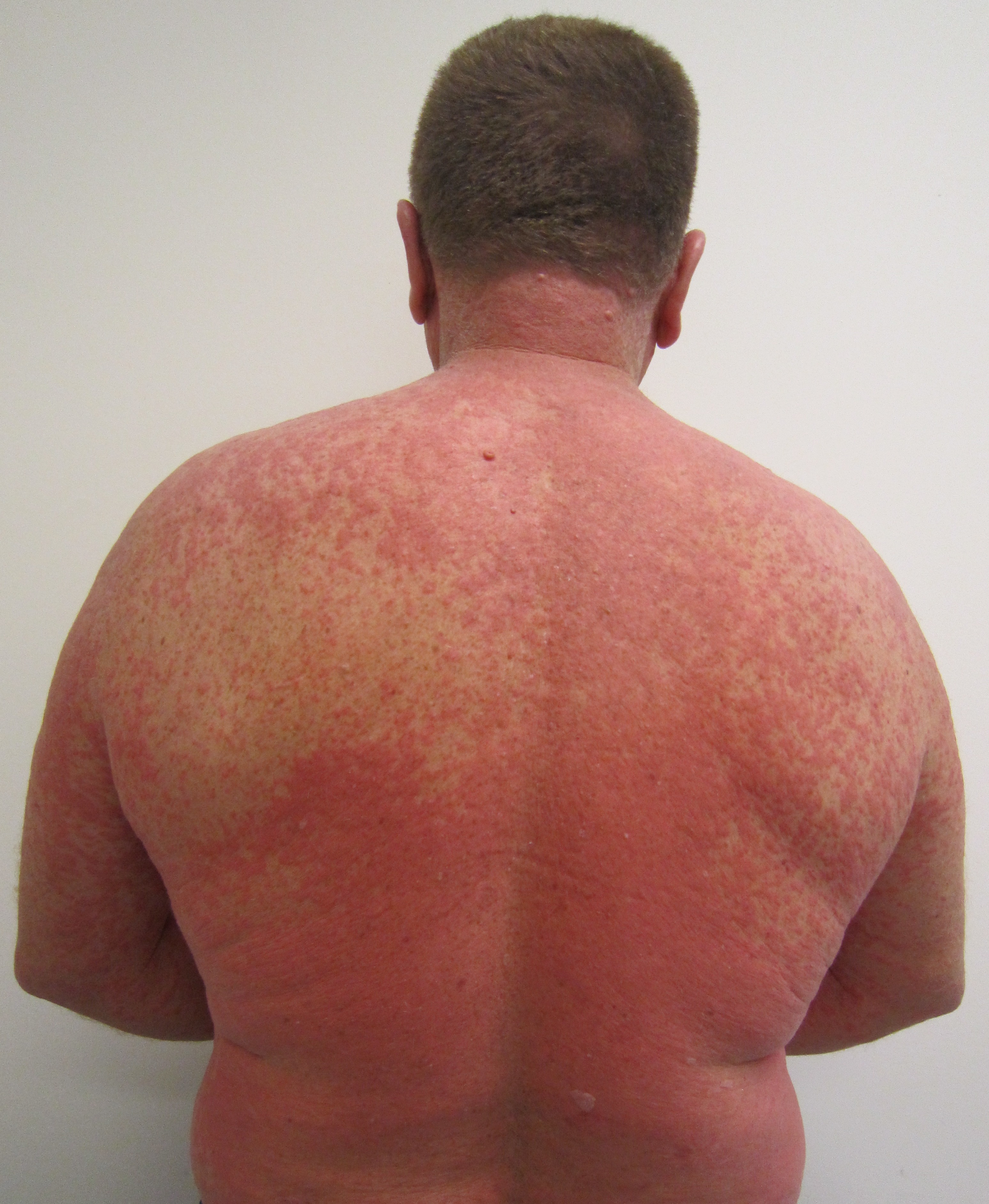
Adverse reactions represent the unintended, often harmful, consequences that can arise from medical treatments, medications, or procedures. These reactions…
Contents
Overview
The concept of unintended harm from medical interventions is as old as medicine itself. Ancient physicians like Hippocrates recognized that treatments could cause illness, a principle later encapsulated in the aphorism 'primum non nocere' – 'first, do no harm.' The systematic study of adverse drug reactions (ADRs) gained significant traction in the 20th century, particularly after tragic events like the thalidomide disaster in the late 1950s and early 1960s, which reportedly led to severe birth defects in thousands of infants. This spurred the development of rigorous drug testing protocols and the establishment of regulatory bodies. The term 'pharmacovigilance' itself was coined in the 1960s, formalizing the discipline dedicated to monitoring drug safety post-market. Early pioneers like Dr. Frances Oldham Kelsey at the FDA played a crucial role in preventing thalidomide's approval in the United States, highlighting the importance of vigilance.
⚙️ How It Works
Adverse reactions can manifest through various biological mechanisms, broadly categorized into Type A (augmented) and Type B (idiosyncratic) reactions. Type A reactions are dose-dependent and predictable, often stemming from exaggerated pharmacological effects of a drug, such as bleeding from anticoagulants like warfarin or hypotension from antihypertensives. Type B reactions, conversely, are unpredictable, not dose-related, and often due to hypersensitivity or immune responses, like penicillin allergies or Stevens-Johnson syndrome. Other classifications include Type C (chronic), Type D (delayed), and Type E (end of use) reactions. The interaction of a drug with an individual's genetic makeup, existing health conditions, and other concurrent medications can significantly influence the likelihood and severity of an adverse event.
📊 Key Facts & Numbers
Globally, adverse drug reactions are a significant public health concern. Estimates suggest that ADRs are responsible for approximately 5% of hospital admissions worldwide, with some studies indicating a higher prevalence in elderly patients and those with multiple comorbidities. In the United States, the CDC reports that medication errors, which encompass ADRs, lead to over 100,000 deaths annually. The economic burden is staggering, with estimates of ADR-related healthcare costs in the U.S. alone reaching tens of billions of dollars each year, potentially exceeding $130 billion according to some analyses. Furthermore, a substantial percentage of these reactions, perhaps up to 30%, are considered preventable through better prescribing practices and patient monitoring.
👥 Key People & Organizations
Key organizations driving the understanding and mitigation of adverse reactions include the World Health Organization (WHO), which maintains the Uppsala Monitoring Centre (UMC) to coordinate global pharmacovigilance efforts. National regulatory agencies like the FDA in the U.S. and the EMA in Europe mandate post-market surveillance and collect reports of ADRs. Pharmaceutical companies themselves are legally obligated to conduct safety monitoring and report suspected ADRs for their products. Leading academic institutions and research centers, such as the Johns Hopkins University's Center for Drug Safety and Effectiveness, contribute vital research into risk factors, detection methods, and prevention strategies. Prominent figures in pharmacovigilance include Klaus Berger and Bruce Goldman, who have contributed to developing methodologies for signal detection and risk assessment.
🌍 Cultural Impact & Influence
The awareness of adverse reactions has profoundly shaped public perception of medicine and healthcare. Media coverage, particularly of high-profile drug failures like thalidomide or the opioid crisis, has fostered a degree of public skepticism and a demand for greater transparency. Patient advocacy groups, such as those focused on rare diseases or specific conditions like autoimmune diseases, often play a crucial role in reporting and raising awareness about under-recognized ADRs. This heightened awareness has also influenced the development of 'black box warnings' on drug labels by regulatory bodies, serving as prominent alerts to healthcare providers and patients about serious potential risks associated with certain medications, impacting prescribing habits and patient education strategies.
⚡ Current State & Latest Developments
Current efforts in pharmacovigilance are increasingly leveraging big data analytics and artificial intelligence to identify potential ADR signals more rapidly and efficiently. Real-world data (RWD) from electronic health records (EHRs), insurance claims, and patient-generated data through mobile health apps are being integrated into safety monitoring systems. The focus is shifting from reactive reporting to proactive risk identification and management. Furthermore, advancements in genomics and pharmacogenomics are paving the way for personalized medicine, aiming to predict which patients are most likely to experience specific ADRs based on their genetic profile, thereby enabling tailored treatment strategies and minimizing harm. The COVID-19 pandemic also accelerated the development and monitoring of vaccines, leading to unprecedented levels of real-time safety data collection and analysis for novel mRNA vaccines.
🤔 Controversies & Debates
A persistent debate revolves around the balance between drug innovation and patient safety. Critics argue that the stringent regulatory processes, while necessary, can stifle the development of potentially life-saving medications, leading to delays in market entry. Conversely, others contend that the current system is insufficient to catch all serious ADRs, pointing to instances where drugs with significant risks were approved and later withdrawn or heavily restricted. The definition and causality assessment of ADRs themselves are also subjects of ongoing discussion, particularly distinguishing between true drug reactions and events that occur coincidentally. The role of off-label prescribing and the challenges in monitoring ADRs in vulnerable populations, such as children and the elderly, remain critical areas of contention.
🔮 Future Outlook & Predictions
The future of managing adverse reactions lies in a more predictive and personalized approach. Pharmacogenomics will likely become standard practice, allowing clinicians to select medications and dosages that are optimized for an individual's genetic makeup, thereby minimizing the risk of adverse events. The integration of wearable technology and continuous health monitoring could provide real-time data on physiological responses to medications, enabling early detection of potential issues. Furthermore, advanced computational models and machine learning algorithms will continue to refine signal detection from vast datasets, identifying rare but serious ADRs much earlier in a drug's lifecycle. Regulatory frameworks are also expected to evolve, potentially incorporating more adaptive approaches to safety monitoring that can respond dynamically to emerging data.
💡 Practical Applications
Adverse reactions are a critical consideration in virtually all aspects of healthcare. For physicians and nurses, understanding potential ADRs is fundamental to safe prescribing and patient management, informing drug selection, dosage adjustments, and patient counseling. In pharmaceutical development, identifying and mitigating ADRs is a core component of drug discovery and clinical trials, influencing go/no-go decisions and labeling requirements. Regulatory agencies use ADR data to issue safety alerts, update prescribing information, and, in severe cases, withdraw drugs from the market. For patients, awareness of potential reactions empowers them to communicate effectively with their healthcare providers and to report any unexpected symptoms, contributing vital information to pharmacovigilance efforts.
Key Facts
- Category
- science
- Type
- topic